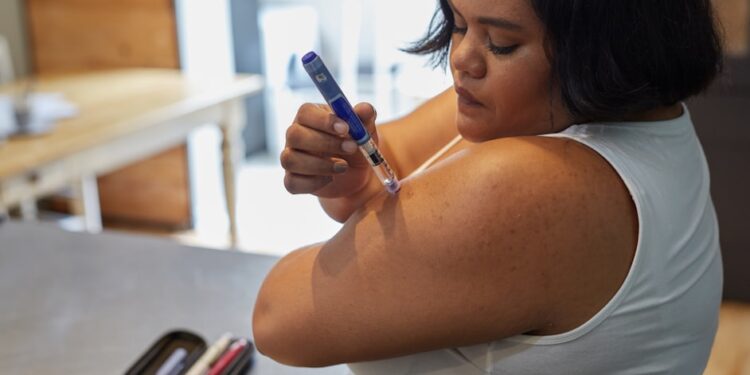
The early signs of insulin resistance in women are quieter and stranger than most people expect. Stubborn belly fat that will not budge on a clean diet. Afternoon crashes that send you hunting for chocolate at 3pm. Skin tags appearing on your neck. Acne flaring after 35. Irregular periods. Hair thinning at the temples. These look like unrelated nuisances. They are often one condition, showing up in the way female physiology handles it.
Insulin resistance develops slowly, often for 10 to 15 years before it registers as prediabetes on a routine blood test. That is a long window of foggy energy, unexplained weight gain, and cycle disruption that most doctors do not recognize because the standard fasting glucose test stays normal until very late in the process.
This guide walks through the early signs of insulin resistance in women that show up well before a diabetes diagnosis, explains why they are different from the signs men get, and covers the lab tests and daily habits that actually move the needle. If you have been told your bloodwork is fine but your body is telling you otherwise, this is the conversation nobody had with you.
- 1 Why the Early Signs of Insulin Resistance in Women Look Different
- 2 Stubborn Belly Fat That Will Not Respond to Diet
- 3 Afternoon Energy Crashes and Sugar Cravings
- 4 Skin Tags, Darkened Skin Patches, and Acne That Shifts
- 5 Irregular Cycles, PCOS, and Fertility Struggles
- 6 Brain Fog and Mood Volatility
- 7 High Fasting Insulin with Normal Fasting Glucose
- 8 Sleep Disruption, Especially Around 3am
- 9 Frequent Hunger and Rapid Weight Regain
- 10 The Perimenopause Acceleration
- 11 What to Do Once You Recognize the Pattern
- 12 Frequently Asked Questions
- 13 Conclusion
Why the Early Signs of Insulin Resistance in Women Look Different

Insulin is the hormone that shepherds glucose from your bloodstream into cells, where it gets burned for energy or stored. When cells become less responsive to insulin’s signal (resistant), the pancreas has to pump out more and more insulin to keep blood sugar in normal range. Fasting glucose stays normal for years. Fasting insulin, however, rises quietly in the background.
Women experience this differently than men for a few overlapping reasons. Estrogen and progesterone both modulate insulin sensitivity. In the luteal phase, in perimenopause, postpartum, and during periods of under-eating, sensitivity drops and the same meal produces a bigger insulin spike. Women also store more fat subcutaneously than men, which masks the classic belly-first appearance of insulin resistance until fairly late. The metabolic dysfunction is happening; it is just distributed differently.
Polycystic ovary syndrome (PCOS), which affects roughly 1 in 10 women, is essentially insulin resistance expressed through the ovaries. Endometriosis, unexplained infertility, and recurrent miscarriage are also associated with insulin signaling problems. This is why the early signs of insulin resistance in women often surface as cycle or skin or hair symptoms long before they surface as weight or blood sugar symptoms.
Stubborn Belly Fat That Will Not Respond to Diet

Of all the early signs of insulin resistance in women, midsection weight gain is the one that shows up most reliably on visual inspection. Visceral fat, the deep fat around organs, is both a cause and a consequence of insulin resistance. It secretes inflammatory signals that worsen the condition while also being the hardest fat to lose. A waist circumference over 35 inches (88 cm), or a waist-to-hip ratio over 0.85, is one of the most reliable early signs of insulin resistance in women, even when BMI is normal.
The tell-tale pattern is weight gain that concentrates around the midsection, especially after a period of stress, poor sleep, or hormonal change. The stubbornness is the key signal. A woman with normal insulin sensitivity usually loses weight on a reasonable deficit within weeks. A woman with insulin resistance often sees the scale barely move for months on the same effort, while feeling hungry, foggy, and tired. That pattern is not willpower. It is metabolism.
Afternoon Energy Crashes and Sugar Cravings

Among the early signs of insulin resistance in women, the 3pm wall is the one almost everyone notices but few connect to the underlying cause. If you feel sharp until 11am and then hit a wall around 2 to 4pm that only a cookie or a coffee can fix, you are likely riding a blood sugar rollercoaster. A lunch high in refined carbs spikes insulin, which drives glucose into storage faster than needed. The resulting dip triggers cortisol to mobilize glucose back up, and your brain registers the rebound as hunger, fog, and sugar craving.
These crashes are among the most common early signs of insulin resistance in women because they appear before any clinical lab is abnormal. They do not happen to people with balanced blood sugar. The fix (30 to 40 grams of protein at each meal, fiber, some healthy fat, and minimal refined carbs) almost always smooths the 3pm wall within a few days, which also confirms the diagnosis by response.
Skin Tags, Darkened Skin Patches, and Acne That Shifts
The skin tells on the metabolism before most other systems do, which makes it one of the clearest early signs of insulin resistance in women. The skin is one of the most underrated windows into metabolic health. Skin tags around the neck, armpits, or groin are strongly linked to elevated insulin. So is acanthosis nigricans, the darkened, velvety patches that show up in the same areas. Both are caused by insulin binding to IGF-1 receptors in skin tissue, which drives abnormal cell growth.
Adult-onset acne or acne that shifts to the jawline and chin after age 30 is also on the list. Insulin drives androgen production in the ovaries, and androgens drive oil production in skin. That is why PCOS and acne so often travel together. If you started breaking out in your 30s after clear skin in your 20s, the skin is often the first place insulin resistance becomes visible.
Thinning hair at the temples or crown, with simultaneous unwanted hair growth on the chin or upper lip, points to the same androgen-insulin loop.
Irregular Cycles, PCOS, and Fertility Struggles
Among the early signs of insulin resistance in women, menstrual irregularity is the one that most often gets written off as “just stress.” Cycles longer than 35 days, skipped periods, very heavy or very light flow, or midcycle spotting can all be downstream of insulin-driven hormonal disruption. The mechanism is androgen excess combined with disrupted ovulation signaling.
Of all the early signs of insulin resistance in women, cycle disruption is the one that most strongly predicts long-term fertility impact, which is why it is worth paying attention to early. PCOS is the extreme of this spectrum, but many women with perfectly normal-looking ultrasounds have the same metabolic profile. If you are trying to conceive and it is taking longer than expected, a fasting insulin and a fasting glucose test, plus a HOMA-IR calculation, is worth asking for. Treating insulin resistance is often the single biggest lever for restoring ovulation, regardless of whether a PCOS diagnosis is on the chart.
Brain Fog and Mood Volatility
Cognitive symptoms are among the most overlooked early signs of insulin resistance in women because they get attributed to stress or hormones. The brain uses about 20 percent of your daily glucose, and it is particularly sensitive to unstable blood sugar. Insulin resistance produces a characteristic fog: fine in the morning, foggy by midafternoon, irritable when meals are delayed, with word-finding problems and short-term memory dips. Many women describe it as “hormonal brain fog” without realizing that the hormone driving it is insulin.
Anxiety, low mood, and emotional reactivity also get worse as insulin resistance progresses, because the cortisol and inflammation that ride along with it affect the same brain circuits. Research connecting insulin resistance to depression has strengthened over the past decade, and in many women, improving insulin sensitivity lifts mood meaningfully within weeks.
For a deeper dive into the neurological side of unstable fuel delivery, see our guide on daily habits to reduce brain fog naturally.
High Fasting Insulin with Normal Fasting Glucose
This is the single most important test most women have never had. Fasting glucose stays normal for 10 to 15 years while fasting insulin rises steadily. A fasting insulin over 10 mIU/L is a concern, over 15 is clearly elevated, and under 6 is optimal. Paired with fasting glucose, a HOMA-IR score above 1.9 suggests meaningful insulin resistance, even in lean, apparently healthy women.
The National Institute of Diabetes and Digestive and Kidney Diseases confirms that insulin resistance precedes measurable glucose abnormalities by many years, which is why asking for fasting insulin (not just A1C and fasting glucose) catches the problem earlier. If your doctor will not order it, many direct-to-consumer labs offer the test for under $30.
Other labs worth watching: triglyceride-to-HDL ratio (above 2.0 is suspicious), uric acid (often elevated), and C-reactive protein for inflammation. These are the early signs of insulin resistance in women that show up on bloodwork before A1C does.
Sleep Disruption, Especially Around 3am
If you fall asleep easily but wake between 2 and 4am and struggle to get back to sleep, blood sugar is often the driver. A late carb-heavy dinner spikes insulin, which later dips blood sugar below baseline. The body responds with cortisol to mobilize glucose, and cortisol at 3am produces exactly the kind of wide-awake, slightly anxious wake-up most women have come to expect with age.
This is one of the most under-recognized early signs of insulin resistance in women, especially in perimenopause, where it gets attributed entirely to hot flashes. The early signs of insulin resistance in women that involve sleep are often the most disruptive to quality of life, which is why addressing them early matters. A small amount of protein before bed (20 grams, a handful of almonds, a tablespoon of nut butter) often resolves the 3am wake-up within two weeks, again confirming the cause by response.
Frequent Hunger and Rapid Weight Regain
Runaway hunger is one of the most frustrating early signs of insulin resistance in women because it feels like a character flaw but is purely biological. Insulin is an appetite regulator. When levels are chronically high, the brain reads it as a sign that fuel is plentiful but not accessible, and responds with hunger, cravings, and lowered resting metabolism. Women with insulin resistance often describe being hungry within two hours of eating, craving sugar specifically, and regaining weight rapidly after any weight loss attempt.
This is not lack of discipline. It is a hormonal feedback loop that defends stored fat. Breaking the loop usually requires targeting insulin specifically, not calories. Lower-carb eating, protein prioritization, strength training, meaningful fasting windows, and better sleep all reduce insulin independently of calorie restriction.
The Perimenopause Acceleration
Perimenopause is when the early signs of insulin resistance in women often become impossible to ignore. If you made it into your late 30s or 40s without obvious metabolic problems and are suddenly gaining belly fat, foggy, not sleeping, and hungry all the time, perimenopause is very likely unmasking insulin resistance that was subclinical before. Estrogen supports insulin sensitivity, and as it begins its irregular decline, the metabolic buffer comes with it.
The Mayo Clinic notes that the menopause transition is associated with weight gain, increased abdominal fat, and a rise in type 2 diabetes risk that is not fully explained by age alone. Catching the early signs of insulin resistance in women during perimenopause, rather than after, changes the long-term trajectory considerably.
What to Do Once You Recognize the Pattern
Reversing insulin resistance is one of the most rewarding interventions in women’s health because the body is still in the reversible phase for years before it becomes diabetes. The habits that move the needle most, in order of impact:
Protein at every meal. 30 to 40 grams, starting at breakfast. Protein reduces the insulin response of mixed meals, preserves muscle (the main glucose sink), and reduces cravings.
Walk after meals. A 10 to 20 minute walk within 30 minutes of eating lowers the postprandial glucose spike by 20 to 30 percent. This is one of the fastest-acting interventions on the list.
Strength training, two to three times weekly. Muscle tissue is the largest consumer of glucose in the body. More muscle means better insulin sensitivity, regardless of weight change.
Prioritize sleep. A single night of five hours of sleep reduces insulin sensitivity the next day by about 25 percent. Chronic short sleep accelerates insulin resistance faster than most dietary changes can fix it.
Reduce refined carbohydrates. Not all carbs, but specifically the refined flours and sugars that produce large insulin spikes. Whole food carbs with fiber (legumes, vegetables, whole fruit) behave very differently.
Consider intermittent eating windows. A 12 to 14 hour overnight fast is plenty to give insulin levels a chance to drop between meals. Extended fasts are unnecessary and often counterproductive for women.
For a complementary morning structure that supports metabolic health, see our guide on morning routine for energy and focus. The overlap with insulin resistance reversal is substantial.
If stubborn weight and fatigue are features of your daily experience, our article on daily habits to boost metabolism after 40 pairs directly with this guide, and the cortisol-driven side of the problem is covered in daily habits to reduce cortisol naturally.
Frequently Asked Questions
What are the first early signs of insulin resistance in women?
The earliest signs typically include stubborn belly fat that will not respond to diet changes, afternoon energy crashes with strong sugar cravings, skin tags around the neck or armpits, irregular menstrual cycles, adult-onset acne (especially on the jawline), and waking between 2 and 4am. These appear long before fasting glucose becomes abnormal.
Can you be insulin resistant and still thin?
Yes. The term is “thin outside, fat inside” (TOFI), and it is more common in women than many clinicians realize. Visceral fat and insulin resistance can develop in people with normal BMI, particularly if diet is high in refined carbohydrates, sleep is poor, or there is a family history of diabetes or PCOS. A fasting insulin test and a HOMA-IR calculation catch this profile that standard BMI-based screening misses.
What is a normal fasting insulin level for women?
Optimal fasting insulin is under 6 mIU/L. A level of 6 to 10 is acceptable but worth watching. Above 10 suggests insulin resistance is developing, and above 15 is clearly elevated. Fasting insulin rises for years before fasting glucose does, which is why it is a more sensitive early test than A1C alone.
How long does it take to reverse insulin resistance naturally?
Meaningful improvement in fasting insulin, HOMA-IR, and energy symptoms is often visible within 6 to 12 weeks of consistent habits (protein prioritization, walking after meals, strength training, better sleep, reduced refined carbs). Full reversal in women who are not yet diabetic typically takes 6 to 12 months. The earlier it is caught, the faster it reverses.
Does PCOS always mean insulin resistance?
Roughly 70 to 80 percent of women with PCOS have insulin resistance, though not all do. The lean PCOS phenotype (normal weight with PCOS symptoms) often still has insulin resistance that requires a fasting insulin test to detect, because standard glucose testing misses it. Treating insulin resistance is one of the most effective interventions for PCOS symptoms, whether body weight is elevated or not.
Conclusion
The early signs of insulin resistance in women are often dismissed as normal aging, hormonal noise, or discipline problems. They are none of those things. They are one condition, expressing itself through skin, cycles, energy, sleep, and slow-motion weight gain, a decade or more before fasting glucose ever registers the problem.
If three or more of the patterns in this article describe your daily life, it is worth asking for a fasting insulin test, a HOMA-IR calculation, and a triglyceride-to-HDL ratio. And it is worth starting the three habits with the biggest return (protein at every meal, a short walk after eating, and strength training two to three times weekly) before waiting for the labs to come back. The pattern is reversible, often dramatically so, when it is caught while it is still just a whisper.
Medical Disclaimer: This article is for educational purposes only and is not intended as medical advice or a substitute for professional diagnosis. The symptoms described can overlap with other medical conditions including thyroid dysfunction, PCOS, perimenopause, and diabetes. Always consult with a qualified healthcare provider before making significant changes to your diet, exercise, or supplement regimen, particularly if you are pregnant, nursing, managing a chronic condition, or taking prescription medications.