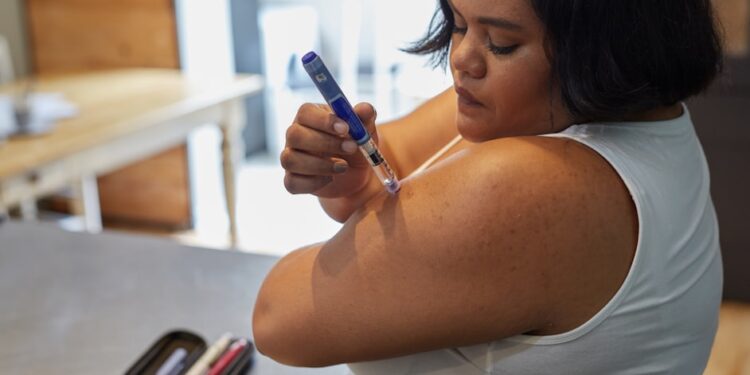
To lose weight with insulin resistance, the standard advice of eat less and move more rarely works, at least not the way it works for people without the condition. If you have been cutting calories, exercising regularly, and still watching the scale refuse to move, insulin resistance may be the reason. Understanding what is happening hormonally, and adjusting your approach accordingly, changes everything.
Insulin resistance affects an estimated 1 in 3 adults in the United States, yet most people discover they have it only after months of frustrating, unexplained weight loss failure. This guide covers why the condition makes fat loss physiologically harder, and exactly how to work around it with specific, actionable strategies backed by current research.
- 1 Why Insulin Resistance Makes Weight Loss So Hard
- 2 Signs You May Have Insulin Resistance
- 3 How to Lose Weight with Insulin Resistance: 7 Proven Strategies
- 3.1 1. Restructure Your Plate Around Protein and Fiber
- 3.2 2. Cut Refined Carbs, Not All Carbs
- 3.3 3. Prioritize Resistance Training Over Cardio
- 3.4 4. Use Meal Timing to Lower Baseline Insulin
- 3.5 5. Fix Sleep and Stress Before Anything Else
- 3.6 6. Consider Time-Restricted Eating or Low-Carb Cycling
- 3.7 7. Discuss Medication Options with Your Doctor
- 4 Best Foods to Eat and Avoid with Insulin Resistance
- 5 Women, PCOS, and Perimenopause: A Harder Battle
- 6 What to Expect Week by Week
- 7 Frequently Asked Questions
- 7.1 Can you lose weight if you have insulin resistance?
- 7.2 What is the best diet to lose weight with insulin resistance?
- 7.3 How long does it take to reverse insulin resistance?
- 7.4 Does intermittent fasting help with insulin resistance?
- 7.5 Is exercise effective for insulin resistance even without weight loss?
- 8 Conclusion
Why Insulin Resistance Makes Weight Loss So Hard

Insulin is the hormone that signals your cells to absorb glucose from the bloodstream and use it for energy. When cells become resistant to that signal, your pancreas compensates by pumping out more and more insulin to get the same effect. The result is chronically elevated insulin levels, and this is where the weight loss problem begins.
High insulin does two things that directly block fat loss. First, it actively suppresses lipolysis, the process your body uses to break down stored fat for fuel. As long as insulin is elevated, your body cannot easily access fat stores regardless of how large a calorie deficit you create. Second, high insulin drives glucose into fat cells for storage rather than into muscle cells for energy use, so excess calories preferentially become fat rather than fuel.
Research published in the National Institutes of Health found that insulin resistance significantly impairs weight loss outcomes in women even when exercise and calorie restriction are applied, because the hormonal environment makes fat oxidation inefficient. A standard calorie deficit that produces a pound of weight loss per week in an insulin-sensitive person may produce almost nothing in someone with significant insulin resistance.
The fat that accumulates with insulin resistance also tends to concentrate in the abdomen. Visceral fat, the fat stored around organs in the belly, is metabolically dangerous because it drives further inflammation, worsens insulin signaling, and creates a self-reinforcing cycle that makes both insulin resistance and weight loss harder over time.
Signs You May Have Insulin Resistance

Insulin resistance does not always produce obvious symptoms, which is why it often goes undiagnosed for years. The most common signs include:
Abdominal weight gain that resists dieting. Fat that accumulates specifically around the midsection, regardless of overall calorie intake, is one of the strongest outward indicators.
Energy crashes after meals. If you consistently feel fatigued, foggy, or drowsy 1 to 2 hours after eating, particularly after carbohydrate-heavy meals, this reflects poor glucose regulation.
Intense carbohydrate cravings. When cells are not getting glucose efficiently, the brain signals for more sugar and refined carbs, driving cravings that feel physically compulsive.
Dark patches of skin. Acanthosis nigricans, patches of darkened skin in the neck creases, armpits, or groin, can indicate elevated insulin levels and is particularly visible in women with PCOS.
Difficulty losing weight despite consistent effort. If your calorie intake and activity level should theoretically produce fat loss but do not, insulin resistance is often the underlying reason.
Diagnosis is confirmed with a fasting insulin test or a glucose tolerance test with insulin levels measured. A fasting insulin above 10 uIU/mL suggests resistance even if fasting glucose is still in the normal range.
How to Lose Weight with Insulin Resistance: 7 Proven Strategies
The key to successfully losing weight with insulin resistance is working with your hormonal environment rather than against it. These strategies directly target the mechanisms that block fat loss in insulin-resistant individuals.
1. Restructure Your Plate Around Protein and Fiber
Protein and fiber are the two most powerful tools for lowering the insulin response to meals. Protein stimulates glucagon, insulin’s counter-hormone, and has a much lower insulin-stimulating effect than carbohydrates. Fiber slows glucose absorption and reduces post-meal insulin spikes.
Practical targets: aim for 30 to 40 grams of protein per meal, and at least 10 grams of fiber per meal from vegetables, legumes, or whole grains. Building every plate around these two macronutrients first, then adding complex carbohydrates in smaller portions, produces a fundamentally different hormonal response than a standard Western eating pattern. This is also why a high-protein breakfast is particularly effective for insulin-resistant women.
2. Cut Refined Carbs, Not All Carbs
Eliminating all carbohydrates is neither necessary nor sustainable for most people. The key distinction is between refined carbohydrates, which cause rapid, large insulin spikes, and slow-digesting complex carbohydrates, which produce a much more gradual insulin response.
Remove: white bread, white rice, pasta, pastries, breakfast cereals, crackers, fruit juice, and anything with added sugar. Replace with: sweet potato, oats, quinoa, lentils, beans, and whole fruit. This shift alone can reduce average daily insulin levels substantially within two to three weeks.
3. Prioritize Resistance Training Over Cardio
Exercise improves insulin sensitivity through two mechanisms: it depletes muscle glycogen stores, creating a demand for glucose that bypasses the normal insulin-signaling pathway, and it increases the density of insulin receptors on muscle cell membranes over time.
Resistance training produces both effects more powerfully than steady-state cardio. Aim for 3 to 4 sessions per week of strength training targeting large muscle groups, particularly legs and back, which are the body’s largest glucose sinks. A 30-minute resistance session can improve insulin sensitivity for up to 24 to 48 hours afterward.
Cardio still has value, particularly low-intensity walking after meals, which can reduce post-meal glucose spikes by 20 to 30 percent. A 10-minute walk after eating is one of the most underrated tools for managing insulin levels.
4. Use Meal Timing to Lower Baseline Insulin
Baseline insulin levels are lowest when you go extended periods without eating. Compressing your eating into a structured window, rather than grazing throughout the day, allows insulin to drop between meals and gives your body more time in the fat-burning state.
A simple approach is to eat within a 10 to 12 hour window and avoid eating 3 hours before bed. This does not require strict intermittent fasting, but it does mean eliminating late-night snacking, which is one of the most insulin-disruptive patterns. For women who want a more structured approach, intermittent fasting for women over 40 explains how to apply time-restricted eating safely.
5. Fix Sleep and Stress Before Anything Else
Sleep deprivation and chronic stress both directly impair insulin sensitivity through cortisol. A single night of poor sleep can reduce insulin sensitivity by 25 percent in healthy adults. In insulin-resistant individuals, the effect compounds quickly.
Cortisol raises blood glucose by stimulating liver glucose production, forcing the pancreas to secrete more insulin to compensate. This creates an insulin spike even without eating. Prioritizing 7 to 8 hours of sleep and adding structured stress reduction, such as 15 minutes of daily low-intensity movement or breathing exercises, are not optional lifestyle upgrades when you are trying to lose weight with insulin resistance. They are mechanically necessary.
6. Consider Time-Restricted Eating or Low-Carb Cycling
For people who have plateaued despite the steps above, two more targeted interventions have strong evidence specifically for insulin resistance. Time-restricted eating within a 16:8 window consistently lowers fasting insulin in clinical studies. Low-carb cycling, where you reduce carbohydrates to under 50 grams on 3 to 4 days per week while eating normally on others, improves insulin sensitivity without the sustainability problems of permanent very-low-carb eating.
If your weight loss has stalled despite consistent effort, the approach outlined in breaking a weight loss plateau addresses the underlying hormonal recalibration strategies in detail.
7. Discuss Medication Options with Your Doctor
For significant insulin resistance that does not respond adequately to lifestyle changes alone, several medications improve insulin sensitivity and support weight loss. Metformin is the most established, reduces liver glucose output, and has a strong safety record. Inositol, particularly myo-inositol, is an evidence-backed supplement that improves insulin signaling, especially in women with PCOS. GLP-1 receptor agonists such as semaglutide are highly effective for insulin resistance and weight loss but require a prescription and medical supervision.
These options are worth discussing with your doctor if you have made consistent lifestyle changes for 12 weeks without adequate results.
Best Foods to Eat and Avoid with Insulin Resistance

Eat more of these:
Non-starchy vegetables (spinach, broccoli, cauliflower, zucchini, peppers) – high fiber, minimal glucose impact. Fatty fish (salmon, sardines, mackerel) – omega-3s reduce inflammation and improve insulin receptor function. Eggs – high protein, zero glycemic impact, keep insulin stable for hours. Legumes (lentils, chickpeas, black beans) – slow-digesting carbs with high fiber and protein. Berries – lowest glycemic index of all fruits, high in antioxidants that reduce oxidative stress. Nuts and seeds – protein plus healthy fats slow glucose absorption. Apple cider vinegar before meals – 1 to 2 tablespoons has been shown in small studies to reduce post-meal glucose spikes by up to 20 percent.
Avoid or minimize these:
Sugary drinks including juice and soda – liquid glucose with no fiber causes the fastest, largest insulin spikes. White bread, pasta, and white rice – rapidly digested, minimal satiety. Breakfast cereals – most are high-sugar even when marketed as healthy. Ultra-processed snack foods – combination of refined starch and seed oils drives inflammation. Alcohol – directly impairs insulin sensitivity and adds empty calories without satiety.
Women, PCOS, and Perimenopause: A Harder Battle
For women, the challenge to lose weight with insulin resistance is compounded by two specific conditions that dramatically increase its prevalence and severity: PCOS and perimenopause.
PCOS and insulin resistance. According to the World Health Organization, polycystic ovary syndrome affects an estimated 10 to 13 percent of women globally, with up to 70 percent of cases undiagnosed. Between 35 and 80 percent of women with PCOS have insulin resistance, with higher rates in those with elevated BMI. Critically, women with PCOS require up to 20 percent fewer calories for weight maintenance compared to women without PCOS, which means standard calorie-deficit recommendations consistently underperform. The elevated insulin drives androgen production, which promotes abdominal fat storage and suppresses fat oxidation, creating a cycle that standard dieting cannot break without addressing the insulin component first.
Perimenopause and menopause. The menopausal transition is characterized by a physiological increase in insulin resistance independent of weight or diet. As estrogen falls, fat distribution shifts from hips and thighs to the abdomen, insulin sensitivity decreases, and the same dietary patterns that maintained weight in your 30s produce steady gain in your 40s and 50s. Research published in the GREM Journal (2024) confirmed that insulin resistance rises significantly during the perimenopausal period and persists through postmenopause, requiring specific dietary and exercise adjustments to manage.
For women in this category, the strategies in this article are not optional modifications but the necessary foundation. Higher protein intake, resistance training, and meal timing control are the three interventions with the strongest evidence for the hormonal environment of perimenopausal insulin resistance.
What to Expect Week by Week
Setting realistic expectations is one of the most important things you can do when trying to lose weight with insulin resistance. Progress is slower than for insulin-sensitive individuals, and the early weeks look different.
Weeks 1 to 2: Bloating and water retention often decrease noticeably as refined carbohydrates are reduced. Scale weight may drop 2 to 4 pounds, mostly water and glycogen, which can be misleading. Hunger patterns begin to shift, particularly if meal timing is being adjusted. Energy may be variable as the body adapts.
Weeks 3 to 4: Insulin levels begin to normalize with consistent dietary changes. Carbohydrate cravings typically reduce. Genuine fat loss begins, though the rate is slower than average, often 0.5 to 0.75 pounds per week at this stage. This is normal and expected, not a sign of failure.
Weeks 5 to 8: Insulin sensitivity improves measurably with consistent resistance training. Energy levels stabilize. Fat loss becomes more visible, particularly around the abdomen, even when the scale moves slowly. Sleep quality often improves, which further accelerates progress through cortisol reduction.
Months 3 to 6: Women who remain consistent through the early adaptation period typically achieve 8 to 15 pounds of fat loss over this timeframe, alongside meaningful improvements in fasting insulin, energy, and body composition. Progress is not linear and plateaus are common at the 6 to 8 week mark, after which adjustments to meal timing or exercise intensity usually restart movement.
Frequently Asked Questions
Can you lose weight if you have insulin resistance?
Yes, but it requires a different approach than standard calorie restriction. Because elevated insulin blocks fat release from cells, reducing insulin levels through dietary restructuring, meal timing, and resistance training is the primary lever. Once insulin levels normalize, fat loss proceeds, though typically at a slower rate than in insulin-sensitive individuals. Expecting the same speed as someone without insulin resistance leads to unnecessary frustration and early quitting.
What is the best diet to lose weight with insulin resistance?
No single diet is universally best, but the most evidence-backed dietary patterns share common principles: high protein (30 to 40g per meal), high fiber (25 to 35g daily), low refined carbohydrates, and minimal added sugar. Both Mediterranean and low-glycemic diets consistently improve insulin sensitivity in clinical studies. The practical key is reducing post-meal insulin spikes by replacing fast-digesting carbohydrates with slower options and pairing all carbohydrate-containing meals with protein and fiber.
How long does it take to reverse insulin resistance?
Meaningful improvement in insulin sensitivity can be measured within 4 to 8 weeks of consistent dietary and exercise changes. Full reversal, where fasting insulin returns to normal ranges, typically takes 3 to 6 months of sustained lifestyle changes. Women with PCOS or significant perimenopausal insulin resistance may find improvement takes longer and requires additional interventions such as inositol supplementation or metformin alongside lifestyle changes.
Does intermittent fasting help with insulin resistance?
Yes. Time-restricted eating consistently lowers fasting insulin levels in clinical studies, often more effectively than calorie restriction alone. The fasting period allows insulin to fall to its lowest baseline, which is when fat oxidation occurs most readily. A 14 to 16 hour eating window is the most studied and practical starting point for insulin-resistant women. The key is not going so long that cortisol spikes undo the benefit, which is why very long fasts are generally not recommended for women managing hormonal imbalances.
Is exercise effective for insulin resistance even without weight loss?
Significantly so. Resistance training improves insulin sensitivity through mechanisms that are entirely independent of weight loss. Building muscle increases the body’s capacity to store and use glucose without insulin, which directly lowers circulating insulin levels. Studies have found that 8 weeks of progressive resistance training improves insulin sensitivity by 25 to 40 percent in insulin-resistant adults, even without significant changes in body weight. This is why exercise is a non-negotiable component of any insulin resistance management plan, not an optional add-on.
Conclusion
Learning to lose weight with insulin resistance means accepting that the standard approach does not apply to your biology. The goal is not simply to eat less but to eat in a way that lowers insulin levels, restores metabolic flexibility, and creates a hormonal environment where fat release is possible. Higher protein, lower refined carbohydrates, consistent resistance training, structured meal timing, and quality sleep are not optional lifestyle upgrades. They are the specific tools that address the specific mechanism blocking your progress.
Progress will be slower than the promises attached to most diets. It will also be more durable. As insulin sensitivity improves, fat loss accelerates, cravings reduce, and energy stabilizes in ways that generic calorie-cutting rarely produces. Give the approach at least 8 weeks before evaluating results.
Medical disclaimer: This article is for informational purposes only and does not constitute medical advice. Insulin resistance is a medical condition that should be evaluated and managed in consultation with a qualified healthcare provider. Do not start or stop any medication, supplement, or restrictive dietary protocol without professional guidance.